CoServ News
Featured Stories
What to expect on your April bill
The weather in March 2024 hit the sweet spot in North Texas – not too hot or too cold. As a result, energy usage should be lower this month.
National Lineman Appreciation Day
This year, we let children write in to tell us why they appreciate CoServ’s electric linemen using words and hand-drawn pictures!
CoServ powers the need for speed at Texas Motor Speedway
Since the grand opening in 1997, CoServ has delivered reliable electricity to the east side of TMS. But there’s much more to the partnership.
Recalculation coming for Fixed Budget Billing
April is a budget billing recalculation month for those on the Fixed Budget Billing plan, meaning the amount due will be adjusted.
What to expect on your March bill
Spring came early to North Texas this year, resulting in lower energy usage for CoServ electric Members and gas Customers.
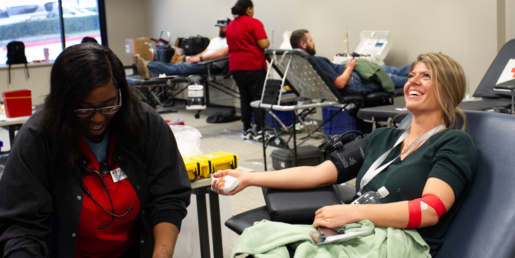
Spring Blood Drive sets multiple records to help American Red Cross
CoServ’s spring blood drive set multiple records for the American Red Cross, collecting 71 total units to help those in need.
Thank the workers who keep natural gas flowing
CoServ gas technicians performing a steel tap into a new regulation station removing a 2-inch line and installing a new 4-inch line allowing for more…
Hard work pays off as CoServ maintains 99.99 percent reliability in 2023
CoServ Members had reliable, uninterrupted electric service 99.99 percent of the time in 2023 with a SAIDI score of 31.4.